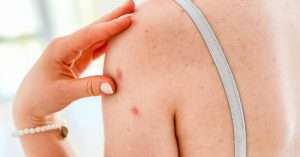
Fungal acne is not the usual acne that we are all familiar with, it is a skin condition called pityrosporum folliculitis. It is one of many types of folliculitis, a skin condition that causes an infection of the hair follicle. It can look like pimples and is often mistaken for acne. For this reason, it’s important to understand what fungal acne looks like and how it develops. Read this article from The Dermo Lab in collaboration with dermatologist and cosmetologist Dr. Dalia Dawood to learn about the symptoms and signs of fungal acne and what you can do to treat and prevent breakouts.
Fungal Acne vs. Normal Acne
Most typical forms of acne are caused by clogged pores. While the source of clogging may vary from person to person (hormones, skin care products, diet, and medications are often blamed), acne itself remains the same. Something clogs the tiny hair follicles in your skin and your skin reacts in the form of red, raised bumps called pimples, which may or may not have a white or black opening.
Fungal acne, on the other hand, has a completely different origin. According to Dr. Dalia Dawood, fungal acne, scientifically known as pittosporum folliculitis, is a type of infection of the hair follicles by a yeast called Malassezia furfur.
Malassezia yeast is a normal inhabitant of our skin, but it can overgrow under certain conditions. In this case, it causes inflammation of hair follicles and can lead to fungal acne.
Dr. Dalia Dawood points out that acne causes blackheads, whiteheads, cysts, and nodules, while fungal acne causes extremely itchy, monomorphic red papules on shoulders, back, chest, arms, and face that are 1-2 mm in size.
What causes fungal acne?
Since overgrowth of Malassezia yeast causes fungal acne, common causes of this condition are situations and environments that promote the rapid growth of the yeast. Dr. Dalia Dawood states that this yeast thrives in a warm, humid environment, which is why it occurs in the summer. It can also appear after treatment with steroids and antibiotics, and it can appear on people with diabetes.
Other situations include:
- Having a high sebaceous gland production
- Frequent sweating, whether due to the climate, exercise, or a health condition
- Not changing into clean clothes after exercise
- Wearing tight, constricting clothing (especially in hot climates)
- Certain diseases or immunosuppressive medications.
Age and gender may also play a role in your risk factors. The disease is most common in teenagers and young men, but it can also affect women.
How is this skin condition diagnosed?
If you think you have symptoms of fungal acne, you may want to see a dermatologist.
Dr. Dalia Dawood indicates that this skin condition is diagnosed clinically by the presence of small, monomorphic, red, highly itchy papules on the shoulders, back, chest, arms, and face.
She adds that a wood lamp can be used which gives a bluish-white fluorescence in the follicular pattern. Microscopic examination after scraping the lesion can also be used to confirm the presence of spores and hyphae.
Fungal acne is often misdiagnosed as regular acne. It is important to distinguish between the two because antibiotic treatment can make the problem worse. If left untreated, fungal acne can persist for many years.
What are the fungal acne treatment options?
Fungal acne is often poorly treated because it looks so much like regular acne. People with this skin condition, unaware of the difference, may treat it with the usual acne treatment options. These treatments are not effective and can worsen the infection.
Treatment for fungal acne has two goals: treating the yeast growth and addressing the underlying cause. If only the yeast growth is treated, fungal acne is likely to recur. Many treatment options can help.
1- Shower more regularly
Depending on the severity of your breakouts, adjusting your lifestyle may be all it takes to remedy fungal acne. If you exercise regularly or have a job that makes you sweat, try showering and changing your clothes right after the gym or work.
This can help remove excess yeast that may have started to grow in the hot, humid environment that develops in sweaty clothes.
2- Wear looser clothing
If you frequently wear tight clothing, the friction and poor air circulation can promote yeast growth on the skin.
Opt for loose, breathable fabrics more regularly to help your skin benefit from good circulation and promote balanced bacterial and fungal growth.
3- Try a body wash
Anti-dandruff shampoos containing zinc pyrithione or selenium sulfide can be used as body washes. Rinse your skin several times a week with these anti-dandruff shampoos.
You may also consider using it regularly to help maintain a healthy balance between the yeast and bacteria on your skin. Leave the shampoo on your skin for several minutes before rinsing it off for best results.
4- Use medical treatments
If lifestyle changes have no effect, the next step is to try a topical treatment. There are a variety of over-the-counter antifungal creams and ointments.
Dr. Dalia Dawood recommends looking for products containing ketoconazole or clotrimazole cream for mild cases. For severe cases, oral antifungals such as fluconazole or itraconazole may be used.
Antibiotics don’t help, and that’s how your doctor can recognize the problem.
How can I prevent it?
The best way to prevent fungal acne is to avoid conditions that promote yeast growth. According to Dr. Dalia Dawood, wearing looser clothes, showering, and changing your clothes after sports or work is helpful.
A balanced diet is another way to help. Fungi like yeast thrive on sugary carbohydrates, so balance your diet with fruits, vegetables, and protein to help discourage growth. You can also use an anti-dandruff shampoo regularly to help maintain a healthy balance of yeast on your skin.
Note from The Dermo Lab
Fungal acne is a type of hair follicle infection caused by an overgrowth of yeast. While the irritation and appearance of fungal acne can be annoying, the cause is usually treated easily and can be prevented with a suitable skin care routine.
It’s important to note that fungal folliculitis does not respond to the usual acne medications, and using these medications can make it worse. Learning to recognize this specific type of skin infection can also help you prevent future breakouts.
If you have tried to treat your suspected fungal acne at home and the rash persists for more than 3 weeks, call your dermatologist.
Last Updated on April 16, 2024